
The Painkillers You Take Could Be the Real Cause of Your Chronic Migraines | Medication Overuse Headache

The Painkillers You Take Could Be the Real Cause of Your Chronic Migraine
|
“If I don’t take Imitrex, I can’t even make it to work.” |
As soon as she woke up, her head throbbed. She takes a triptan two or three times a week, sometimes even four times. And almost every day, she adds Tylenol or an NSAID. That afternoon, the fluorescent lights felt unusually harsh, and her heart pounded with noise. Her sleep was shallow and broken.
|
Medication Use Pattern (Summary) • Triptans (e.g., Imitrex) approx. 10 times per month • Analgesics (NSAID/acetaminophen) almost daily • History of taking tranquilizers (variable dosage) |
Her records reveal a pattern. Unilateral pulsating pain follows visual aura (flashing lights, blurred vision), accompanied by photophobia, phonophobia, and nausea. Triptan use is approximately 10 times a month, and milder analgesics are taken “almost daily.” Neurological examinations at a university hospital three years ago were normal. However, recently, the medication has become less effective. She finds herself reaching for medication more often and sooner.
|
Like a malfunctioning fire alarm, the pain network easily triggers even with minor stimuli. |
Here's an important question.
“Does the medication eliminate the headache, or does it perpetuate it?”
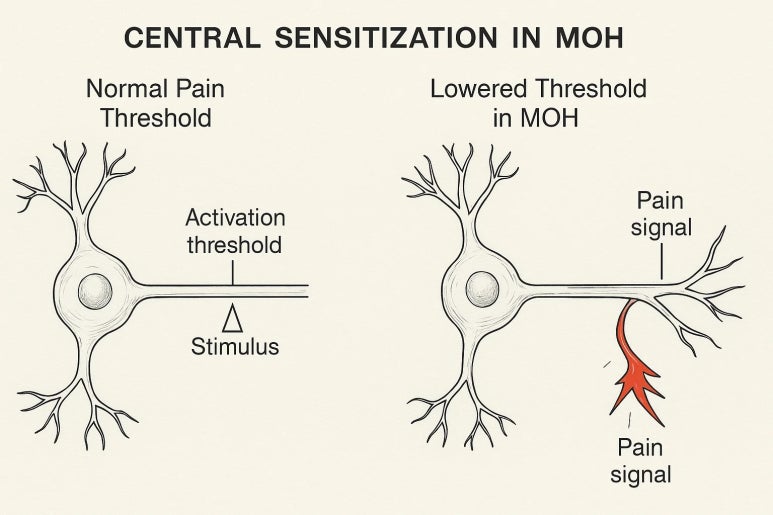
Frequent use of triptans and NSAIDs leads to medication overuse headache (MOH). In a sensitized pain network, the threshold of the serotonin and neuroinflammation axis is lowered, causing it to easily activate. Stopping the medication brings on a surge of headaches, while taking it only provides temporary relief.
In terms of Traditional Korean Medicine (TKM), prolonged tension and sleep deprivation cause Liver Yang to ascend (肝陽上亢, ganyang-sanggak), while a weakened Spleen and Stomach allow Phlegm-Dampness to surge upwards (痰濁上擾, tam-tak-sang-yo). Epigastric tenderness, loss of appetite, and bloating are its traces. On nights with shallow sleep and a rapid heart rate, headaches are more likely to occur the next morning. Viewing this simply as a "problem of the head" leads to superficial prescriptions.
|
Contraindications/Exclusion Criteria (Safety Confirmation) • Neurological imaging/examinations normal 3 years ago • No focal neurological warning signs (e.g., acute hemiplegia, speech disorder, sudden vision changes) |
Thus, the treatment revolves around two axes. First, strategies to reduce medication dependence. Acute phase medications are gradually reduced based on their 'total weekly dosage.' A migraine trigger diary is kept to numerically track the correlation between sleep, diet, stress patterns, and attacks.
Second, prescriptions that address the root cause. Initially, Banha Baekchul Cheonma Tang (半夏白朮天麻湯) is primarily used to clear Phlegm-Dampness and strengthen the Spleen and Stomach. If upward heat (上熱, sang-yeol) and Qi stagnation (氣滯, gi-che) are pronounced, a small amount of Chai Hu (柴胡) and Huang Qin (黃芩) is added to temper the upward surge. As the frequency and intensity decrease, Gami Gwi Bi Tang (加味歸脾湯) is administered to nourish the Heart and Spleen, restoring sleep depth. If menopausal upward heat and emotional fluctuations persist, Gami Soyo San (加味逍遙散) is used to soothe the autonomic nervous system.
|
Treatment Protocol (Summary) 1) Initial Stage: Banha Baekchul Cheonma Tang (半夏白朮天麻湯) ± Chai Hu (柴胡)·Huang Qin (黃芩) (Eliminates Phlegm-Dampness, strengthens Spleen and Stomach, alleviates upward heat) 2) Mid Stage: Gami Gwi Bi Tang (加味歸脾湯) ± Gastrodia (天麻, cheonma)·Uncaria (鈎藤, gudeung) (Stabilizes sleep and emotions, suppresses recurrence) 3) Chronic Stage: Gami Soyo San (加味逍遙散) ± Uncaria (鈎藤, gudeung)·Gastrodia (天麻, cheonma)·Moutan Cortex (牧丹皮, mokdanpi)·Gardenia (梔子, chija) (Alleviates upward heat and emotional fluctuations) |
|
Caution (Tapering Principles) • Triptans/analgesics should be gradually reduced based on total weekly dosage — do not discontinue abruptly. • Do not arbitrarily reduce tranquilizers; if withdrawal symptoms or worsening occur, adjust immediately with a medical professional. |
However, one differential diagnosis is always kept open. If this pain is not truly MOH, the 'baseline frequency' of pain will not significantly change during triptan reduction, and the pattern will remain the same even with improvements in sleep and digestion. In such cases, other variables such as cervical muscle tension, temporomandibular joint dysfunction, anemia, thyroid issues, and drug interactions are examined more precisely.
|
Lifestyle and Dietary Tips • Go to bed before 11 PM, limit afternoon caffeine, consistent two meals a day • 10–15 minutes of bright light immediately after waking + 20–30 minutes of low-intensity aerobic exercise • During an attack: dark room, quiet, cold compress / Regularly: warm compress on trapezius and shoulder girdle • Diet: Avoid trigger foods such as cheese, processed meats, wine, chocolate |
The conclusion is simple: Manage medication, but do not depend on it. Reduce the hypersensitivity of the headache network (serotonin and neuroinflammation axis), restore the digestive function of the Spleen and Stomach (eliminate Phlegm-Dampness), and re-establish sleep rhythm. The goal is not a 'body that can endure without medication,' but a 'body that has increasingly more days without needing medication.' This change is first observed in the weekly medication frequency and attack diary.
|
Record Checklist (Answer with Data) • Total weekly dosage (triptans/analgesics), number of attack days·peak intensity (0–10) • Aura-to-attack interval (minutes), sleep duration·number of nighttime awakenings • Digestion discomfort score (0–10), correlation with trigger foods/menstrual cycle/overtime work/weather |
Applying this to a real schedule makes it clearer. Morning fasting, stress of preparing for work, hurriedly consumed coffee, and skipping breakfast increase the likelihood of an attack on the same morning. Eating lunch late and quickly getting up combines with delayed gastric emptying and gut-brain axis stimulation, reigniting the headache. Conversely, on days with more than 7 hours of sound sleep the night before, avoiding overeating at dinner, and disconnecting from screens two hours before bedtime, the attack intensity is lower.
Translating the TKM framework into modern language, it reads as follows: Liver Yang Ascending (肝陽上亢, ganyang-sanggak) corresponds to sympathetic nervous system overactivity and distorted stress hormone rhythms. Phlegm-Dampness Surging Upwards (痰濁上擾, tam-tak-sang-yo) corresponds to increased intestinal permeability and micro-inflammatory substances circulating and contributing to central sensitization. Formulas like Banha Baekchul Cheonma Tang (半夏白朮天麻湯) manage stomach dampness and phlegm, reducing 'noise' from peripheral input, while Gami Gwi Bi Tang (加味歸脾湯) helps correct the stability of sleep-memory-emotion circuits (hippocampus-ACC).
|
The goal is not 'to endure without medication,' but 'a body that has increasingly more days without needing medication.' |
