
Best Foods for Irritable Bowel Syndrome | "My Stomach Hurts, I Need to Rush to the Bathroom"

“My stomach hurts, and I urgently need to go to the bathroom” | Irritable Bowel Syndrome in Office Workers in their 30s
Have you ever had to rush to the bathroom during an important meeting or work due to frequent abdominal pain and diarrhea?
There have likely been many days when you had to cancel plans or hesitate to eat out because of unpredictable abdominal discomfort.
As late-night work and stress accumulated, your gut likely became even more sensitive, perhaps leading to a vicious cycle where you missed out on important moments in life.
|
Many 30-something office workers I see in my clinic often confess, "My stomach suddenly hurts so much I break into a cold sweat," or "My stomach rumbled like thunder during an important meeting, and it was so embarrassing." I deeply empathize with their constant anxiety, not knowing what to eat or what to avoid. They often lose their vitality, not from a simple stomachache, but from a type of pain where all their nerves seem focused solely on their gut. |
Irritable Bowel Syndrome (IBS) is a very common gastrointestinal disorder affecting approximately 11-14.1% of the global population.
Its prevalence is particularly high among 30-something office workers in today's high-stress society.
This condition goes beyond simple indigestion, severely impacting patients' quality of life.
According to research, IBS leads to reduced sleep quality, employment instability, social activity limitations, and even mental health issues like anxiety and depression, causing suffering comparable to other severe chronic illnesses.
Our gut is so closely connected to the brain that it's often called the "second brain."
This gut-brain axis is highly sensitive to stress and is a major cause of worsening IBS symptoms. It can lead to changes in gut motility, increased visceral hypersensitivity, and an imbalance in the gut microbiota, thereby exacerbating IBS symptoms.
Fluctuations in stress hormones like cortisol also directly impact the gut.
Ultimately, stress management is a crucial key to IBS treatment and must be considered alongside dietary management.
Dietary Management: The Hidden Clue to Irritable Bowel Syndrome

I recall the story of Jihoon (a pseudonym), an office worker in his 30s who recently visited my clinic.
He said he lost sleep and focus due to recurrent abdominal pain and diarrhea leading up to an important presentation.
He expressed his frustration, saying, "Even though it's food I usually eat, my symptoms get worse on particularly stressful days. I don't know what to eat or how to eat."
He was unaware of the "pattern of discomfort" hidden in his diet.
The very process of finding clues about which foods irritated his gut was difficult.
|
Jihoon (a pseudonym) was completely unaware of how the cereal and milk he ate every morning, or the Americano he drank after lunch, affected him. The spicy delivery food he ate while working late into the night also likely put further strain on his gut. I advised Jihoon to "talk to his gut." I suggested he start by meticulously recording the small "clues" — what foods caused his gut to complain of discomfort — without missing any. I emphasized the importance of carefully documenting the food he consumed and his body's reactions to it. |
Our gut constantly reacts to information from external food.
Some foods send peaceful messages to the gut, aiding digestion, while others irritate the intestinal lining, trigger inflammatory responses, and cause discomfort.
Precisely identifying these "patterns of discomfort" is the first step in dietary management.
Low-FODMAP Diet: The Journey to Building Your Own Gut Filter
|
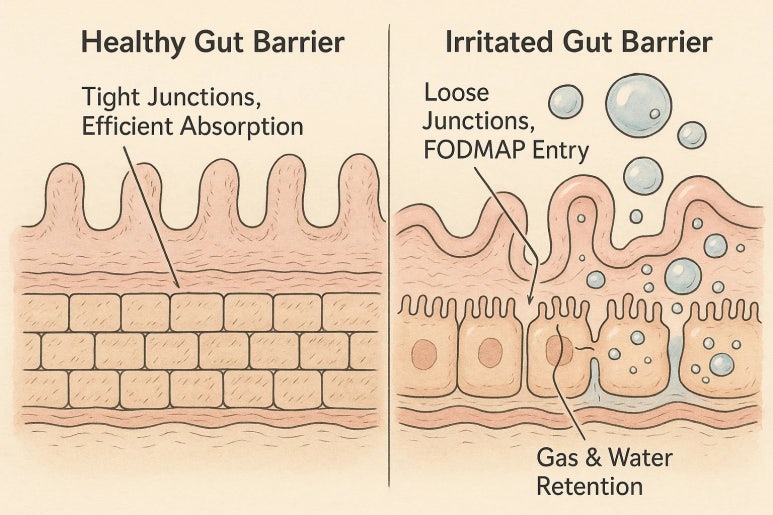
I often use the analogy of a "gut filter" with my IBS patients. Our gut lining, like a fine filter, should absorb good nutrients and filter out harmful substances. However, in some cases, this filter becomes loose or overreacts to certain components, causing undigested carbohydrates (FODMAPs) to ferment in the gut, leading to excessive gas or drawing in water, which results in abdominal pain and diarrhea. In such situations, a low-FODMAP diet is an effective way to tighten this filter and reduce the burden on the gut. FODMAP is an acronym for Fermentable Oligosaccharides, Disaccharides, Monosaccharides, and Polyols, which collectively refer to carbohydrates that are poorly absorbed in the small intestine and easily fermented in the large intestine. Temporarily restricting these high-FODMAP foods can significantly help stabilize the gut environment and alleviate uncomfortable symptoms. |
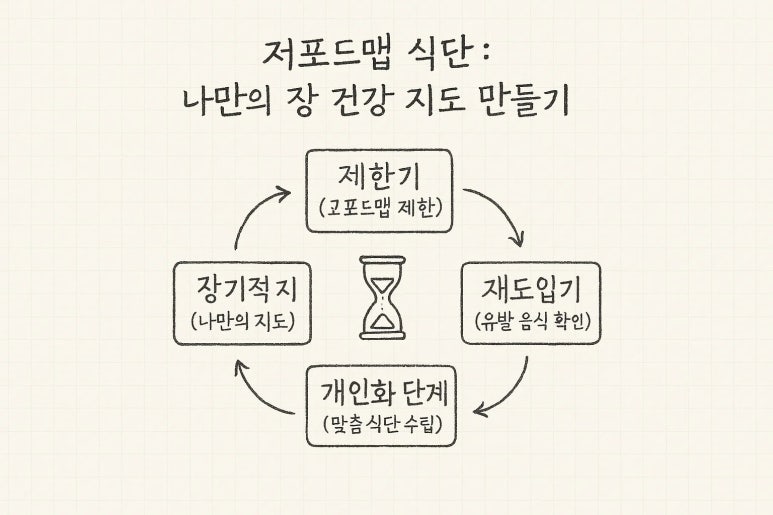
The low-FODMAP diet typically proceeds in three phases.
First is the elimination phase.
For the initial 2-6 weeks, high-FODMAP foods such as apples, garlic, onions, and dairy products are strictly limited to give the gut a rest and observe symptom changes.
Second is the reintroduction phase.
Once symptoms improve, restricted foods are reintroduced one by one, in small amounts, to identify which foods trigger discomfort.
This phase is crucial for discovering your specific food trigger patterns.
Third is the personalization phase.
In this phase, trigger foods identified during the reintroduction phase are adjusted to a suitable level for the individual, establishing a long-term sustainable diet.
Through this process, many patients, like Jihoon (a pseudonym), came to understand for themselves which foods are detrimental and which are beneficial.
Keeping a daily food diary is a critical clue in uncovering these patterns.
By meticulously recording consumed foods and subsequent symptoms (e.g., intensity of abdominal pain, presence of diarrhea/constipation, bloating), you create your own "gut health map."
This map goes beyond a simple diet plan; it empowers you to understand and control your own body.
Your Personalized Gut Health Diet: How to Begin?
For those embarking on the journey of dietary management, I'd like to offer some practical tips.
I hope these tips serve as small milestones on your path to gut health.
|
For those starting their dietary management journey, I recommend utilizing natural seasonings and herbs. While garlic and onions are high-FODMAP foods, you can enhance flavor with low-FODMAP ingredients like ginger, the green parts of spring onions, and various herbs. Furthermore, consistency in meal times is crucial. Irregular eating can disrupt the gut and exacerbate symptoms, so try to establish a habit of eating at set times whenever possible. Adequate hydration is essential for digestive health. I particularly recommend water or caffeine-free herbal teas; peppermint, ginger, and chamomile teas can help soothe the gut and alleviate stress. Peppermint relaxes intestinal smooth muscles, reducing abdominal pain and cramps; ginger can alleviate nausea; and chamomile is useful for reducing stress-related symptoms due to its calming effects. As another approach to gut health, considering probiotic supplements can also be beneficial. A healthy gut microbial environment can positively impact gut function. Finally, stress management is as important as diet. Efforts to find peace of mind through meditation, regular exercise, and sufficient sleep are necessary. Conscious efforts must be made to stabilize the gut-brain axis. |
A Partnered Journey to Understanding Your Gut
|
While a low-FODMAP diet is undoubtedly an effective approach, it is ultimately a temporary "exploration" process. Since high-FODMAP foods often contain important nutrients, long-term, unconditional restriction can lead to the risk of nutritional imbalance. Furthermore, the types and amounts of FODMAPs that individuals react to vary greatly, making it crucial to seek guidance from healthcare professionals or dietitians specializing in digestive disorders to find a personalized diet. It is not advisable to excessively restrict your diet based solely on your own judgment or to conclude it's ineffective and give up. If symptoms worsen or new discomfort arises, always consult a professional for an accurate diagnosis and advice. Remember that hasty judgments can actually harm your gut health. |
Irritable Bowel Syndrome is a discomforting and painful condition, but I always tell my patients, "My gut is talking to me."
By listening to its voice, responding sensitively to small changes, and consistently mapping out your own "gut health map," you can certainly regain a comfortable daily life and efficient work performance.
On this journey, I sincerely hope you find healthcare professionals who meticulously care for your entire body, fostering a healthy partnership, even if it's not with me.
Until the day each of your guts feels comfortable, I will be here to listen, support, and encourage you.
