
Why do you get an upset stomach when you eat cold food?

A Glass of Iced Latte: Why Does My Stomach Go Haywire That Evening?
3 PM, a cold sip.
Around 5 PM, my stomach slowly tightens, with the first pain hitting at 7 PM.
Two trips to the bathroom that night, one in the morning the next day.
“On days I drink warm tea, I'm perfectly fine.”
Tests are always normal, but the results differ when the temperature changes—this is the starting point of the story.
When cold liquid enters, the intestinal barrier's sensory threshold lowers, and peristalsis becomes erratic.
At the moment the stomach should accept and expand, it instead tends toward contraction, leading to bloating.
Peripheral blood vessels momentarily constrict, and the mucosal defense line also weakens.
For sensitive individuals—those with IBS/functional dyspepsia, unstable gut microbiota, or low basal metabolism—this change
is amplified into abdominal pain, bloating, and loose stools.
Even if it's the same 220ml, 4°C and lukewarm water are different events inside the body.
There are many labels: IBS, functional dyspepsia, primary dysmenorrhea.
Each label uses medication (anti-diarrheals, digestive aids, NSAIDs) to reduce the flare-up.
But if the same scene repeats every time, what we've missed is the operating principle.
Here, we see it this way: Temperature Homeostasis Vulnerable Type.
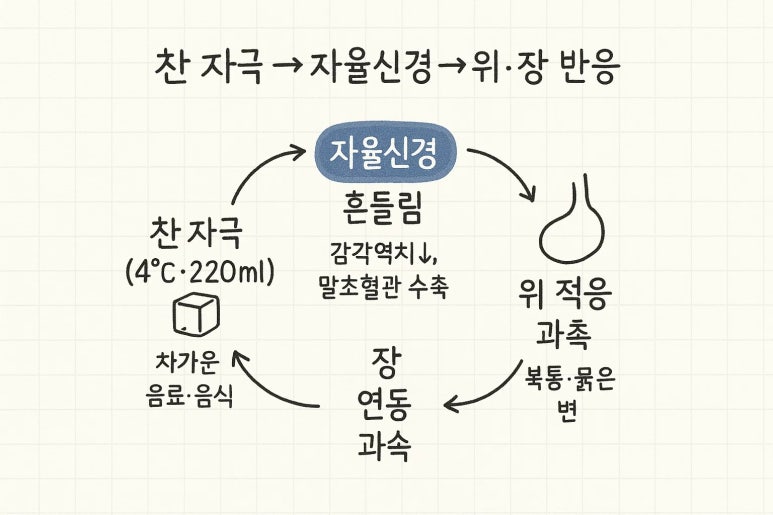
Cold stimulus → Autonomic nervous system instability → Reduced gastric adaptation/Accelerated intestinal peristalsis →
Decreased lower abdominal blood flow + Predominance of pain-transmitting substances.
If individual variables like lactose intolerance, caffeine, and lack of sleep are added to this,
a chain reaction of abdominal pain, diarrhea, and menstrual cramps is completed every evening.
Instead of changing the labels, let's try changing the model.
In the language of Korean traditional medicine, it's Spleen-Stomach Cold Deficiency (Bi-Wi-Heo-Han) and Cold-induced Blood Stasis (Han-Eung-Eo-Hyeol).
If ice chips fall into a weak stove with weak digestive embers, the flame dies out, and only smoke remains.
In the language of Western medicine, it's decreased sensory nerve threshold, smooth muscle hypercontraction, reduced local blood flow,
and in some cases, intestinal barrier vulnerability (tight junction instability).
The two languages take different paths but meet at the same place.
Therefore, the direction of intervention is clear—to strengthen the digestive "embers" and promote blood flow.
Food warm, drinks lukewarm, abdomen with warmth.
If necessary, traditional Korean herbal medicine that warms the Spleen and Stomach (Bi-Wi) (e.g., Ijung-tang, Hyangsaryukkunjatang) is prescribed,
and for menstrual cramps, prescriptions that aid warmth and circulation are tailored.
This is not a "forbidden for life" list, but rather a training to re-learn the temperature and timing that your digestive "embers" can handle.
Let's start with a 5-line daily log:
Time / What was eaten & Temperature / Stomach sensation / Bowel movements / Mood.
- Water and tea lukewarm, 1.5L a day, frequently and in small sips.
- Vegetables and proteins lightly warmed, refrigerated desserts at room temperature for 10 minutes.
- Morning and evening abdominal warm compress for 15 minutes (20 minutes before and after menstruation).
- Coffee slowly after a meal. If iced is necessary, reduce the amount by half.
- Record 'cold events' like 4°C, 220ml and compare them with a lukewarm control.
- If you open your notebook after 3 days, you will see the language of temperature your body speaks.
- From then on, it's not "cold = absolute evil" but "a choice that prioritizes your digestive 'embers'."
